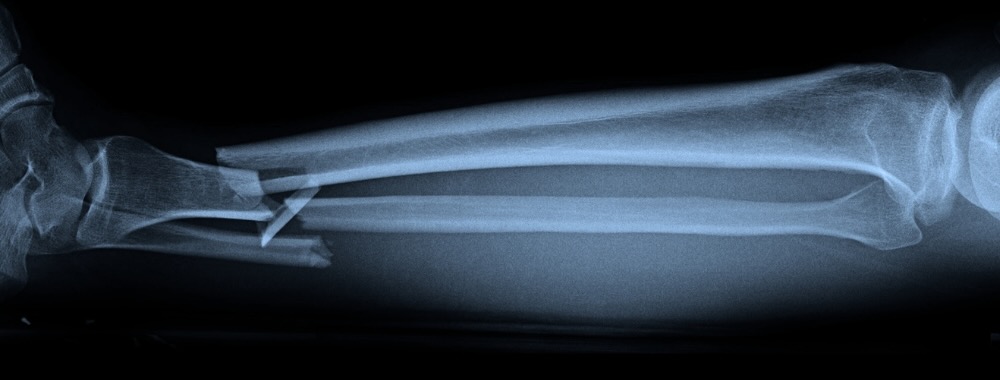
Most of us know that bones need calcium to stay strong, but few people stop to think about the actual structure or what keeps them healthy over a lifetime.
Bones do more than support muscle – they are dynamic, specialized tissue that constantly adapt, repair, and communicate with nearly every other system in the body. They store minerals, produce hormones, house bone marrow for blood cell production, and interact with our immune system.
Understanding the structure and function of bones provides insight into how they grow, heal, and respond to extreme challenges – like the creation of new bone during limb lengthening procedures.
Bone Structure and Function
Bones are complex. At the macro level, cortical bone (compact bone) forms the dense outer shell of the skeleton, giving it strength and rigidity. The inner cancellous bone (spongy bone) has a porous, lattice-like structure that makes bones lighter yet supportive. (Fun fact: spongy bone is also where blood cells are produced.)
Zooming in on the microstructure, bones consist of an interwoven matrix of collagen and minerals (like calcium and phosphate) that harden and provide rigidity. Osteoblasts (bone-building cells) produce collagen and help deposit minerals, while osteoclasts (bone-resorbing cells) break down old or damaged bone. We don’t realize it’s happening, but bones undergo constant remodeling to maintain their strength, repair tiny injuries, and adapt to mechanical stresses throughout our lives.
Bones are hard, but they aren’t sealed off from the rest of the body, and they require a harmonious interplay of other systems. The endocrine system helps regulate bone formation and calcium balance. The immune system releases signaling molecules called cytokines that can influence bone remodeling. The circulatory system delivers oxygen, nutrients, and hormones to bone tissue. Meanwhile, the gastrointestinal tract and kidneys regulate mineral absorption and excretion, affecting bone density.
Bones also give back. Bone marrow is the birthplace of nearly all blood cells, including the white blood cells that power your immune system. Bones also act as a storage reservoir, holding minerals like calcium, phosphorus, and magnesium and releasing them when other organs need them. Even fat stored in the marrow produces hormones that help regulate metabolism. They hold us up in more ways than one.
The Biology of Bone Healing
Distraction osteogenesis is the process of creating new bone to correct limb length differences or deformities. Surgeons divide the bone, stabilize it with an external or internal device, and gradually separate the divided ends with mechanical tension. As the separation occurs, the body lays down new bone in between the gap. Limb lengthening represents one of the highest anabolic demands placed on bone in orthopedic surgery because the body must build substantial new bone mass, not just repair a small area as in a traumatic fracture.
Bone is a living, constantly remodeling tissue. It stores minerals, interacts with hormones, and communicates with the immune system; during limb lengthening, every one of those systems has to work overtime. Also, the liver, kidneys, gastrointestinal tract, and immune system all influence the body’s ability to form healthy regenerate bone. Forming new bone can become less efficient if any of those systems is undernourished or overstressed.
In the lengthening phase, structural tissue is formed. During the consolidation phase, mineralization and strengthening occurs. Both phases depend on:
- Micronutrients as building blocks and catalysts
- A healthy immune system without excessive inflammation response
- Adequate blood circulation for oxygen and nutrient delivery
- Sufficient protein and caloric intake to meet heightened metabolic demand
Unlike a traumatic fracture, limb lengthening is a controlled injury, but the process of regeneration is similar. An inflammatory phase starts the process, releasing signaling molecules called cytokines (including IL-1 and IL-6), which act like biochemical “alerts.” These signals draw in mesenchymal stem cells, which are immature cells that can turn into osteoblasts (bone-forming cells). These cells begin producing collagen and early bone matrix, creating the initial framework for new tissue.
In limb lengthening, once the short waiting period after surgery (the latency phase) passes, the distraction phase begins, where the bones are slowly pulled apart by a few millimeters each day.
As the bone is gradually pulled apart, the body fills the gap with soft, fibrous tissue. Because the stretch happens a little at a time, the collagen fibers line up in the direction of the pull, giving the new bone a sense of orientation. Minerals start to settle into the initial framework, and the soft tissue transforms into woven bone – a rough, early form of new bone. Over time, it strengthens and reorganizes into more mature bone.
Once the desired length is reached, the body enters the consolidation phase, shifting from forming new tissue to strengthening it. Minerals are added, the bone becomes denser, and the body begins reshaping and reinforcing it based on movement. Because the bone responds to pressure by becoming stronger, weight-bearing and mechanical loading are especially important during this stage. A controlled increase of physical activity also helps reduce bone loss in the untouched (native) bone.
Supporting Bone Growth
Bone strength peaks in early adulthood, typically in the late 20s to early 30s, and adequate nutrition provides the raw building materials bones need to grow and mitigate density loss as we age.
Calcium is the primary mineral for bone hardening and density; vitamin D enables calcium absorption. Magnesium helps activate vitamin D and supports collagen formation, while vitamin K2 guides calcium to the bones. Protein supplies amino acids that form the collagen matrix. Zinc, vitamin C, and other trace minerals assist with collagen synthesis, immune regulation, and bone cell function.
When you get to the physical therapy phase of healing, exercise and mechanical loading are just as critical as nutritional intake. Bones respond to impact through a process called mechanotransduction, where physical forces stimulate growth and strengthening. Weight-bearing exercises and resistance training (with the guidance of a physical therapist) create impact stress that encourages bone formation, maintains density, and reduces the risk of fractures. During limb lengthening, controlled mechanical stimulation is vital for both regenerate and native bone.
Limb lengthening is a remarkable demonstration of the body’s capacity to regenerate and heal, and at Premier Limb Lengthening Institute, patients receive guidance on both surgical technique and the lifestyle factors that optimize bone regeneration – every aspect is designed to support the body’s incredible ability to form new bone.