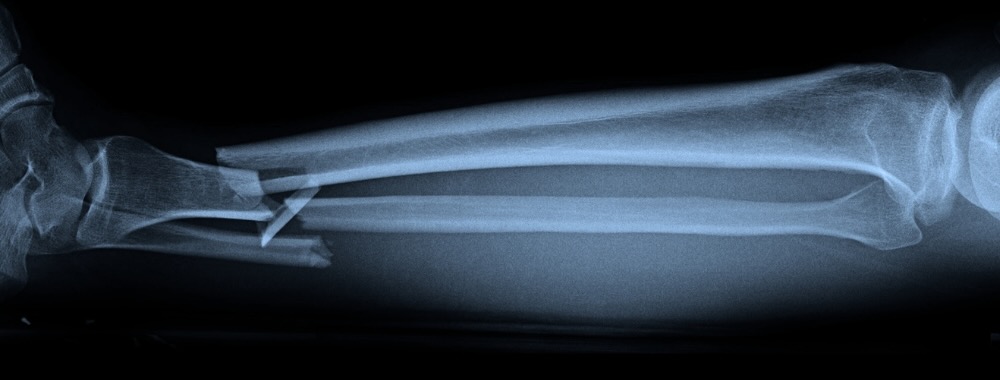
People pursue limb lengthening for various reasons: to correct limb discrepancies caused by congenital conditions or diseases like rickets; to enhance proportion and symmetry; or to restore mobility after severe fractures or bone trauma.
The surgery itself relies on cutting-edge orthopedic techniques, and successful recovery depends just as heavily on a patient’s dedication, particularly to physical therapy (PT). Stretching, strengthening, and retraining muscles and joints, as well as following pre- and post-surgical protocols, determine the resulting mobility and range of motion.
Anatomy of Limb Lengthening
Limb lengthening fundamentally (and obviously) changes the musculoskeletal structure. The procedure begins with an osteotomy – a controlled cut in the bone. Through either an internal or external fixation device, the two bone ends are gradually separated, allowing new bone tissue (called the regenerate) to form in the gap.
But the bone isn’t the only physical structure adapting. As the bone grows longer, all the muscles, tendons, nerves, and blood vessels must stretch and remodel. This puts stress on soft tissues and can cause temporary tightness or discomfort.
- The muscles lengthen under tension and can lose flexibility or strength if not actively stretched and conditioned.
- The joints experience increased mechanical stress and altered alignment, putting them at risk of stiffness or contractures. (A joint contracture is a condition where the muscles, tendons, or other tissues around a joint tighten or shorten, leading to reduced movement and flexibility.)
- The nerves are stretched along with the limb and may become compressed or inflamed, causing them to become irritated if soft tissues don’t lengthen evenly.
- The blood vessels elongate and adjust to new spatial relationships within the limb, so they have to adapt to increased length and pressure changes.
Because every structure has to adjust in synchrony, supervised physical therapy is essential to maintain range of motion and prevent permanent complications.
The Healing Process
Limb lengthening occurs in two overlapping stages: the distraction phase and the consolidation phase.
Distraction Phase: This begins after a latency period post-surgery, once the initial healing starts. The device, either an external fixator or internal nail, is adjusted daily, typically 0.75–1 mm per day, to gradually separate the bone ends. As they separate, the body fills in the gap with new bone tissue – the regenerate. During this stage, soft tissue tightness, pain, and swelling are most pronounced, and daily physical therapy helps offset these effects.
Consolidation Phase: Once the desired length is achieved, adjustments stop, allowing the new bone to harden and mature. This phase can last several months – about twice as long as the distraction period. Physical therapy remains crucial for retraining balance, strength, and gait mechanics while the bone regains full stability.
Throughout both phases, and even before surgery, nutrition, circulation, and activity level all affect the healing process. Patients are advised, based on personal health history, to eat a high-protein diet and to take calcium, vitamin D, and mineral supplements; avoid nicotine, which constricts blood flow and slows bone growth; and follow the activity and weight-bearing guidelines set by the surgical team.
Recovery and Physical Therapy
If surgery is the blueprint, physical therapy is the construction crew; surgery sets the framework, PT integrates that framework with surrounding tissues into functional strength, coordination, and mobility. Inconsistency with rehab and at-home exercises increases the risk of complications like joint stiffness, nerve irritation, muscle contractures, or even palsy. (Muscular contracture is when muscles become permanently shortened and/or tightened, leading to reduced flexibility and difficulty in movement.)
Early Mobilization and Positioning
Physical therapy begins within days after surgery. Getting a head start on appropriate movement prevents joint stiffness and promotes circulation. In this phase, patients learn:
- Proper limb positioning to reduce swelling and prevent deformities.
- How to transfer safely from bed to chair and use assistive devices like crutches or walkers.
- Techniques for sleeping, sitting, and traveling that protect the limb and avoid unnecessary discomfort.
Even simple ankle pumps or isometric contractions (tightening muscles without moving the joint) can help prevent blood clots and maintain muscle tone in the early stages of healing.
Range of Motion (ROM) Exercises
Maintaining joint mobility and all of the structures associated with it is the primary focus of limb lengthening rehabilitation. Therapists target the joints above and below the lengthened bone so that as the bone lengthens, the soft tissues stretch evenly along with it. Regular stretching and tailored range of motion exercises prevent:
- Muscle contractures, such as tightness in the calf or hamstrings.
- Joint subluxation or dislocation, which can occur when imbalanced muscle tension pulls a joint out of alignment.
- Nerve irritation, which can arise from uneven tissue tension.
Sessions in the office, as well as at home, become a way of life, with up to five appointments per week. Between visits, a home exercise program is established to sustain progress.
Strengthening and Functional Retraining
As the new bone consolidates and anatomical structures begin to synchronize and align, therapy shifts toward rebuilding strength, balance, and coordination. Muscles that have been stretched during lengthening may lose efficiency and need to relearn proper activation patterns.
This stage of physical therapy includes:
- Progressive resistance training to rebuild strength without overloading the healing bone.
- Weight-bearing exercises (once cleared by the surgeon) to stimulate bone remodeling and improve density.
- Gait training, which teaches proper walking mechanics and posture, helps patients regain natural movement and confidence.
This is an arduous process, and restoring function requires patience, persistence, and a carefully guided rehabilitation plan that strengthens the body as it adapts to its new proportions.
Preventing Complications
Physical therapy can also be thought of as a preventative measure – patients who skip or minimize PT are at higher risk for permanent issues like nerve palsy, early arthritis, and dislocation.1 Therapists are trained to spot early warning signs, including tightness, asymmetry, and abnormal pain, so that recovery protocols and treatments can be adjusted before minor issues become major setbacks.
Every limb lengthening case is unique, and every body is different, so physical therapy plans are customized based on the bone segment being lengthened and the type of device used (external fixator vs. internal nail), as well as the patient’s age and overall health. A close partnership with the surgeon is non-negotiable to adjust treatment intensity and frequency throughout recovery. It’s a team effort, both in the clinic and at home, between the care teams and the patient.
Recovery timelines vary, and for most patients, the entire process, from surgery through rehabilitation, can take 6 to 12 months, depending on the amount of length gained and individual healing rates. Progress may feel slow, but with diligence, most patients regain full range of motion and function.
Healthy Sidekicks
Physical therapy and recovery are complemented by lifestyle and behavioral factors that can either accelerate or hinder the healing process. Limb lengthening is physically demanding and emotionally taxing. Regular attendance and compliance with home exercises are key predictors of successful outcomes, but so are the modalities a patient chooses that help them stay motivated through long recovery phases. Anything from behavioral therapy sessions to mindfulness and meditation practices can help stave off boredom when laid up or frustration when physical therapy becomes a challenge.
Dietary choices that support both bone regeneration and muscle strength, as well as overall emotional health, are equally important. Eating whole, unprocessed foods like fruits, vegetables, grains, nuts, and fatty fish can support emotional balance by providing essential nutrients that influence mood and brain health. At the same time, limiting processed foods and refined sugars while incorporating probiotics and fiber can boost gut health, which is linked to improved mental well-being.
Limb lengthening is one of modern medicine’s most remarkable reconstructive procedures, but its success depends on the patient’s partnership in recovery. Bones may grow through technology, but muscles, joints, and confidence grow through movement, commitment, and guided therapy.
At Premier Limb Lengthening Institute, we specialize in comprehensive care that starts with pre-operative assessments all the way through full rehabilitation. Learn more about our limb lengthening programs or request a consultation today.
- Bhave, A., Baker, E., & Campbell, M. (2024). Physical therapy during limb lengthening and deformity correction: Principles and techniques. In S. Sabharwal & C. A. Iobst (Eds.), Pediatric lower limb deformities (pp. 363–382). Springer. https://doi.org/10.1007/978-3-031-55767-5_19.